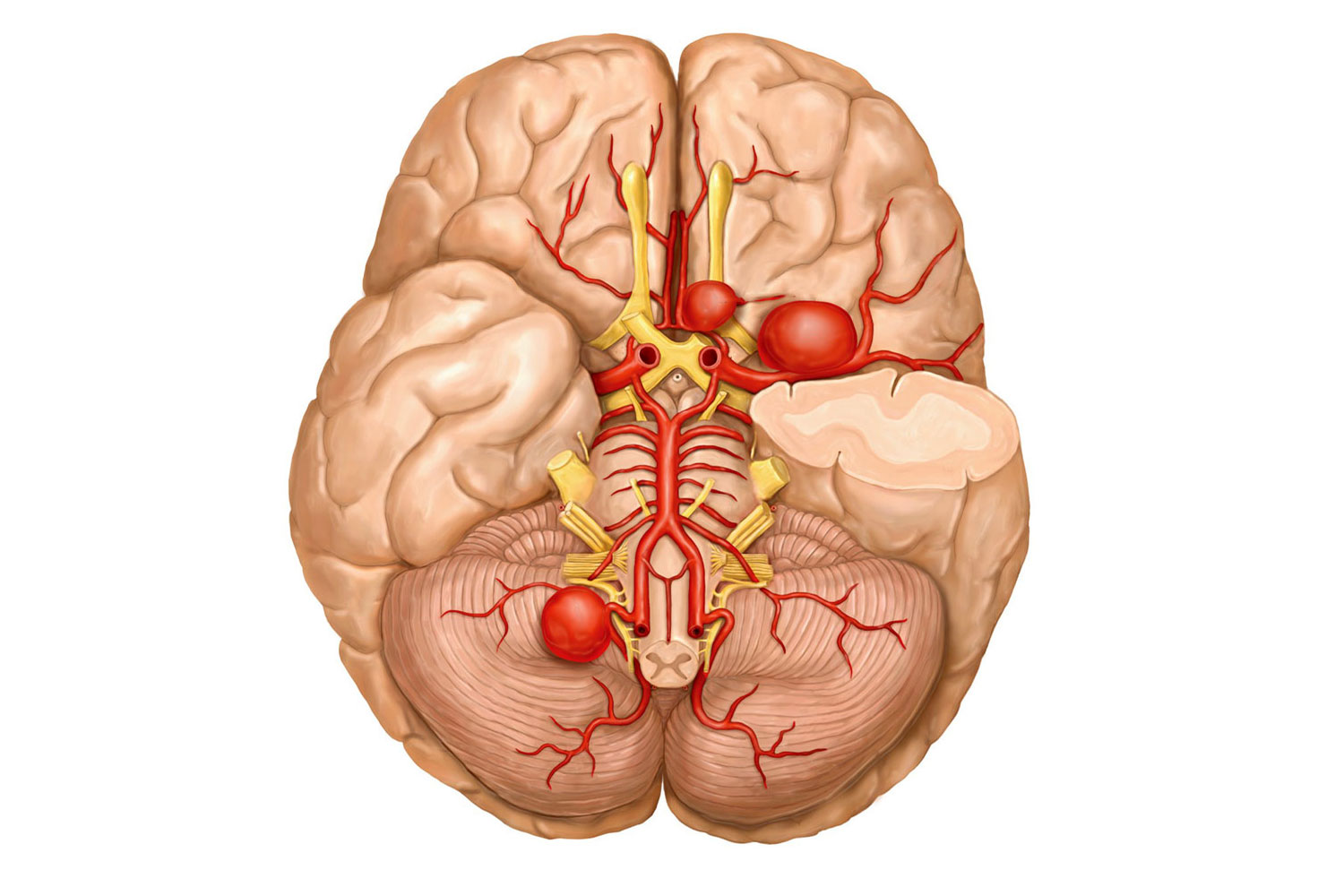
A cavernoma, additionally called cavernous angioma, is a vascular malformation in the brain. The blood vessels are extraordinarily dilated and resemble “little caverns” (for this reason the name) and are clustered together in the form of a tiny round. 3 symptoms are characteristic of a cavernoma: an abrupt neurological deficit, a seizure, or a slow neurological degeneration. These are typically associated with bleeding from the cavernoma, its development, or adjustments in the microcirculation. Its discovery is, more often than not, lucky, and it typically needs a normal follow-up. You can treat this illness with the help of telehealth psychiatry solutions.
Definition as well as Signs
What is Brain Cavernoma?
A cerebral cavernoma is a malformation of the brain’s blood system: the vessels are extraordinarily expanded. In the majority of instances, this anomaly does not include any signs. Sometimes neurological problems (frustrations, obscured vision, and so on) are present.
The number of individuals with this malformation is tough to assess. In particular, due to the fact that a cavernoma is commonly asymptomatic, several individuals are unaware that they have one. According to different research on the subject, the variety of carriers of an analytical cavernoma is approximated between 1 in 200 and 1 in 1000.
A cavernoma affects men and women equally, regardless of their beginning. It typically demonstrates between the ages of 20 and 40 but can also bring about signs and symptoms in childhood or adolescence.
The specific beginning of this vascular malformation is still unclear. We recognize that it is a local anomaly in the advancement of the vessels. Undoubtedly, a cavernoma contains tiny vessels (veins) very dilated, twisted, and also grouped. A cavernoma resembles a round of small, intertwined vessels. Its dimension differs from some millimeters to a number of centimeters.
20% of cerebral cavernomas are domestic forms. Simply put, the malformation is connected with a genetic anomaly that is passed on from generation to generation. The genetics associated with cerebral cavernoma are CCM1, CCM2, and CCM3. These familial forms usually result in the presence of a number of cavernomas. They carry a better danger of issues.
To understand! We can approximately think about genetics as codes for creating healthy proteins. These are essential elements since they add to each cell’s proper functioning and, consequently, more normally of the body.
What Symptoms?
In the huge bulk of cases, particularly almost 90%, the analytical cavernoma is asymptomatic and continues to be quiet. It is then commonly uncovered by coincidence during an MRI (Magnetic Resonance Imaging) for another health problem.
In the staying 10% of situations, the cavernoma is the reason for numerous signs and symptoms. The initial takes place between 20 and 40 years of age. They can lead to epileptic seizures (approximately 70% of instances), frustrations, or other neurological problems (vision disruption, sensitivity disorder in the limbs, etc.). Symptoms differ from client to individual and rely on the number of cavernomas, dimensions, and location.
A lot more rarely, some people may sometimes display non-neurological symptoms, including red areas on the skin and asymptomatic malformations of the blood vessels in the retina. This type of sign is more likely to influence individuals with the familial kind of the condition.
When they exist, signs may schedule either to the cavernoma itself or to the blood loss created. The wall surfaces of cavernomas are thin and fragile, so they damage quickly, causing an effusion of blood, damaging the affected mind frameworks. Nevertheless, also in the occurrence of a rupture, the blood loss is little. Hence, loss of consciousness or coma is very remarkable. A raising dimension cavernoma can occasionally press the mind areas surrounding it and create neurological problems. Ultimately, epilepsy is linked to the inflammation of particular parts of the brain in contact with the cavernoma.
Diagnostic
Mind Imaging
( MRI) Magnetic vibration imaging of the brain is the gold standard for the medical diagnosis of analytical cavernomas. The gradient echo series (T2 *) is the most sensitive for recognizing cavernomas because of its high sensitivity for detecting bleeding traces in mind cells. MRI likewise makes it possible to make the diagnosis yet to date the bleeding and keep track of the advancement of the cavernoma (s) and highlight a connected venous developmental abnormality.
A classification right into 4 classifications has been recommended. It is based on an MRI of the cavernoma (hyperintense, hypointense) on various series (T1, T2, slope echo). Per kind corresponds info concerning the features of the cavernoma (type I: current blood loss, kind II: heterogeneous lesions with blood loss and thrombosis of differing ages, type III: old blood loss, kind IV: aspect stimulating a cavernoma in the process of the constitution).
The follow-up studies of familial cavernomas have validated the vibrant nature of these malformations in mind imaging. The development of cavernomas can result in new lesions or adjustments in their characteristics (especially their dimension). The demo of endothelial expansion at the perimeter of vascular dental caries suggests that angiogenesis sensations can boost the volume of certain cavernomas.
Vessel Imaging.
Cavernomas are not pictured with angiography methods (CT angiography, magnetic vibration angiography, or analytical arteriography) due to the fact that the circulation within the “caverns” (dental caries composing the cavernoma) is done at low circulation, and the vessels are feeding the malformation. They are extremely tiny sizes. Often imaging of the mind vessels is necessary to dismiss an additional sort of vascular malformation. This examination often discloses a developmental venous abnormality related to the cavernoma.
Genetic Medical diagnosis.
The recognition of CCM genetics today makes it technically possible to evaluate these 3 genetics in health center practice. In the unlimited majority of cases, the mutations determined to result in an early quit codon’s look or partial or total deletion of among the 3 CCM genetics.
The testing level of sensitivity in a subject with familial adenomatosis is about 94% (see above), while it is just 57% for a sporadic instance with multiple lesions.
Once the mutation has been determined in an individual, the test’s sensitivity level gets to 100% for his relatives.
The decision to carry out a hereditary examination must be preceded by an initial analysis of this test’s real advantage, particularly when it comes to an asymptomatic subject. These examinations’ sign appears to be variable and differs in different situations (see next phase).
What Development?
Among patients with asymptomatic single cerebral cavernoma, a minority will certainly take eventually to provide with neurological signs and symptoms.
People that have signed may either maintain, or even regress, or intensify with time.
The evolution of a cavernoma depends mainly on its risk of bleeding and its area. A cavernoma is not a precancerous sore, so there is no risk of cancerization or infect the rest of the body to fret about.